You face real risks when combining supplements with medications. About 34.3% of adults in the United States use dietary supplements alongside prescription medications, and supplement interactions medications can affect your health in serious ways. Cardiac symptoms—palpitations, chest pain, and tachycardia—often result from interactions, especially with weight-loss products. Swallowing problems and abdominal pain also appear often. You should always share your full list of supplements and medications with your healthcare provider to protect your safety. The risk of unsupervised mixing increases if you do not consult a healthcare provider.
Medical Disclaimer: This article provides information for educational purposes only. You should always consult your healthcare provider before making decisions about supplements or medications.
Key Takeaways
Always tell your healthcare provider about all supplements and medications you take to avoid dangerous interactions.
Supplements can change how your medications work, making them less effective or causing harmful side effects.
Herbal supplements like St. John’s Wort and Ginkgo Biloba can cause serious drug interactions, especially with heart and blood-thinning medications.
Certain vitamins and minerals, such as calcium and vitamin K, can affect how your body absorbs or responds to medications.
Use trusted drug interaction checkers online before starting new supplements or medications to spot potential risks.
Keep an updated list of all your supplements and medications and share it with your healthcare providers regularly.
Watch for signs of interactions like unusual bleeding, heart changes, mood shifts, or allergic reactions and seek medical help if needed.
Store your supplements and medications properly in a cool, dry place and dispose of expired products safely to maintain their effectiveness.
Supplement Interactions Medications Overview
What Are Interactions?
You may hear the term “drug interactions” often, but what does it mean for your health? Drug interactions happen when two or more substances—such as medications, supplements, foods, or drinks—affect each other’s actions in your body. According to the FDA and NIH, these reactions can change how effective or safe a medication is. Supplements are not just harmless extras. They can act like drugs and cause real changes in how your body handles medications. You face supplement interactions medications risks not only with prescription drugs but also with over-the-counter products and even foods.
Tip: Always tell your healthcare provider about every supplement, medication, and even herbal tea you use. This helps prevent unexpected interactions.
Why Safety Matters
You want your medications and supplements to help, not harm. Drug interactions can make a medication less effective or cause dangerous side effects. Some interactions may increase the risk of bleeding, heart problems, or even life-threatening reactions. The FDA warns that dietary supplements can have strong effects and may interfere with medications or medical procedures. You should care about supplement interactions medications because the risk is real. Even common food-drug interactions, like grapefruit juice with certain heart medications, can cause serious problems. You need to understand these risks to protect your health and safety.
Here are some reasons why safety matters:
Drug interactions can lead to treatment failure or unexpected side effects.
Supplements may change how your body absorbs, breaks down, or removes medications.
Some foods and supplements can block or boost the effects of your medication.
Drug-drug interactions and drug-supplement interactions can happen at any age.
How Drug Interactions Happen
Drug interactions occur through two main pathways:
Pharmacokinetic interactions: These change how your body absorbs, distributes, metabolizes, or eliminates a medication. For example, some supplements affect enzymes like cytochrome P450 (CYP3A4), which handle about 80% of prescribed drugs. If a supplement blocks or speeds up these enzymes, your medication may not work as expected.
Pharmacodynamic interactions: These happen when a supplement or medication changes the way another drug works in your body. The effects may add up or cancel each other out, which can be dangerous.
You also need to watch for supplement and over-the-counter medication risks. Foods can play a big role in interactions. For example:
Calcium-rich foods can lower the absorption of some antibiotics.
Foods high in vitamin K, like spinach, can reduce the effect of blood thinners.
Grapefruit juice can block enzymes and change drug levels in your body.
Note: Always follow medication directions and talk to your healthcare provider about potential interactions. This helps you avoid unwanted side effects and keeps your treatment safe.
You face supplement interactions medications risks every day, whether you take prescription drugs, OTC medications, or dietary supplements. By understanding how drug interactions happen, you can lower your risk and keep your health on track.
Common Drug Interactions
You face many risks when you combine supplements with medications. Some drug interactions can cause harmful side effects or even life-threatening problems. You need to know about common drug interactions, especially if you take high-risk medication combinations or have chronic condition medication interactions. Below, you will find the most important types of interactions to watch for.
Herbal Supplements
Herbal supplements often seem safe, but they can cause severe drug interactions. Many people do not realize that herbs can change how your body handles medication. Some herbs affect enzymes in your liver, which can change drug levels in your blood. This can lead to dangerous outcomes, especially with drugs that have a narrow safety margin.
St. John’s Wort
St. John’s Wort is one of the most common herbal supplements linked to serious drug interactions. It can lower the effectiveness of many medications by speeding up how your body breaks them down. You should avoid St. John’s Wort if you take drugs for depression, birth control, HIV/AIDS, or organ transplants. This herb can also interact with blood thinners and heart medications, leading to severe drug interactions.
Herbal Supplement | Drugs Frequently Interacted With (Number of Cases) |
|---|---|
St. John’s Wort | Cyclosporin (54), Oral contraceptives (12), Antidepressants (9), Warfarin (7), Digoxin (13), Clopidogrel (6), Indinavir (8), Irinotecan (5), Antipsychotics (3), Tacrolimus (1), Anesthetic (1) |
You can see that St. John’s Wort interacts with many drugs, including those for the heart, immune system, and mental health. These drug interactions can cause treatment failure or dangerous side effects.
Ginkgo Biloba
Ginkgo biloba is another herbal supplement that can cause harmful side effects. It increases the risk of bleeding when you take it with blood thinners like warfarin or aspirin. Ginkgo can also interact with seizure medications and antidepressants. If you use ginkgo, you should tell your doctor, especially if you take medication for your heart or brain.
Echinacea
Echinacea is popular for boosting the immune system, but it can interact with medications that affect the liver. This supplement may change how your body processes drugs for infections, seizures, or cholesterol. You should be careful if you use echinacea with other medications, as the risk of drug interactions increases.
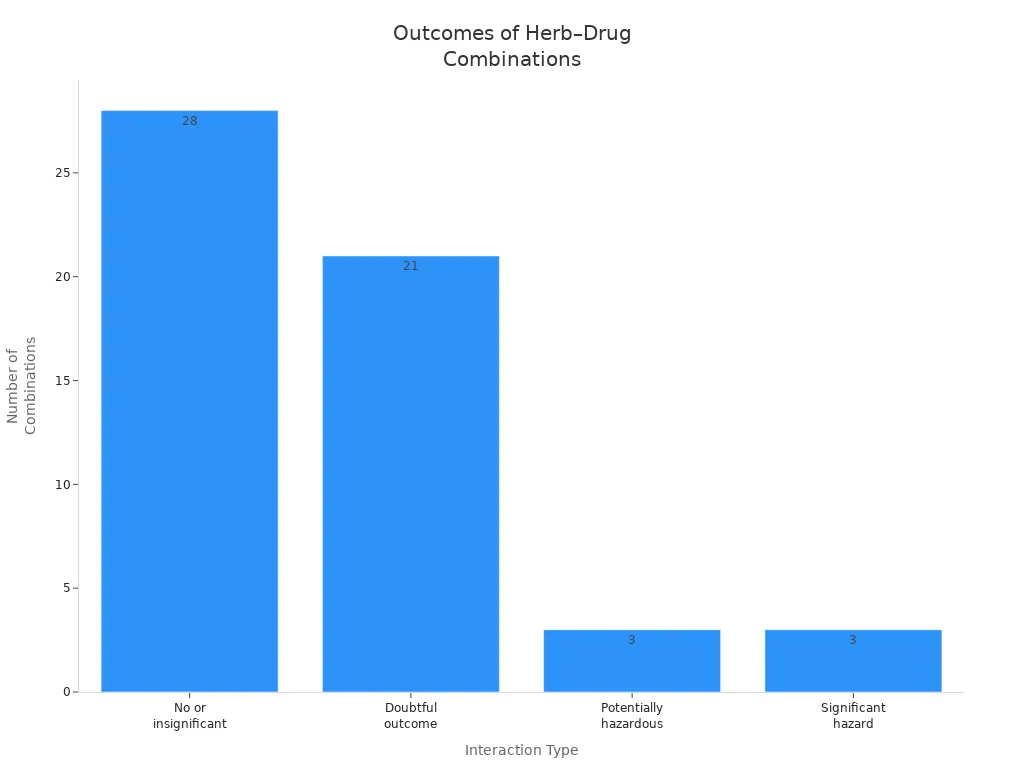
Note: About one-third of older adults who use herbal supplements with prescription drugs face potential interactions. Many of these combinations can lead to harmful side effects or reduce the effectiveness of your medication.
Vitamins and Minerals
Vitamins and minerals are important for health, but they can also cause drug interactions. You may think these supplements are always safe, but they can change how your medication works.
Calcium
Calcium supplements can block the absorption of many medications. If you take calcium with certain antibiotics, thyroid medicine, or HIV drugs, your body may not absorb the medication well. This can make your treatment less effective.
Medication Category | Specific Medications | Notes |
|---|---|---|
HIV Medicines | Bictegravir, Dolutegravir, Elvitegravir, Raltegravir | Calcium affects absorption |
Thyroid Medicine | Levothyroxine | Interaction affects absorption |
Lithium | Lithium | Interaction concerns |
Fluoroquinolones | Ciprofloxacin, Levofloxacin, Moxifloxacin, Ofloxacin | Calcium may reduce effectiveness |
Bisphosphonates | Alendronate, Ibandronate, Risedronate | Calcium affects absorption |
Tetracyclines | Doxycycline, Minocycline, Omadacycline, Sarecycline, Tetracycline | Calcium reduces absorption |
Digoxin | Digoxin | Interaction possible |
You should always tell your healthcare provider if you take calcium, especially if you use any of these medications.
Vitamin K
Vitamin K plays a key role in blood clotting. If you take warfarin or other blood thinners, eating foods high in vitamin K or taking vitamin K supplements can lower the drug’s effect. This can increase your risk of blood clots or stroke. You need to keep your vitamin K intake steady and let your doctor know about any changes.
Magnesium
Magnesium supplements can also cause drug interactions. They can block the absorption of antibiotics and some heart medications. If you take magnesium with digoxin or certain blood pressure drugs, you may face harmful side effects or reduced drug effectiveness.
Tip: More than half of US adults take dietary supplements with prescription drugs. Older adults and people with many medications have a higher risk of drug interactions.
Other Supplements
Some other supplements can also cause drug interactions, especially with heart medications and blood thinners.
Fish Oil
Fish oil is popular for heart health, but it can interact with blood thinners and antiplatelet drugs. Fish oil can increase the effect of these medications, raising your risk of bleeding. Studies show that fish oil does not usually cause more bleeding on its own, but it can have a stronger effect when combined with drugs like aspirin or warfarin. If you take fish oil and blood thinners together, your doctor may need to monitor you more closely.
Fish oil can enhance the anticoagulant effect of warfarin and antiplatelet drugs.
Most studies do not show a big increase in bleeding, but you should still be careful.
If you need surgery, your doctor may ask you to stop fish oil a few days before.
Melatonin
Melatonin helps with sleep, but it can interact with medications for blood pressure, diabetes, and depression. Melatonin may change how your body processes these drugs, leading to either stronger or weaker effects. You should talk to your doctor before using melatonin if you take medication for chronic conditions.
Alert: Drug interactions can happen with any supplement, not just herbal products. Always check with your healthcare provider before starting a new supplement, especially if you take medication for a chronic condition.
Table: Supplements and Blood Thinner Interactions
Supplement | Interaction with Warfarin | Effect on Patient |
|---|---|---|
Garlic | Causes platelet inhibition | Increases bleeding risk |
Ginger | Inhibits thromboxane synthetase | Prolongs bleeding time |
Ginkgo | Increases International Normalized Ratio (INR) | Enhances blood thinning effect |
Ginseng | May reduce warfarin effectiveness | Decreases anticoagulant effect |
Vitamin E | Blood thinning effects, especially in Vitamin K deficiency | Increases bleeding risk |
Alfalfa | Significant interaction (mechanism not detailed) | Alters warfarin effect |
Grapefruit | Significant interaction (mechanism not detailed) | Alters warfarin metabolism |
St. John’s Wort | Significant interaction (mechanism not detailed) | Alters warfarin metabolism |
You need to watch for common drug interactions if you take blood thinners or heart medications. These drug interactions can lead to harmful side effects, such as bleeding or blood clots.
Remember: Drug interactions are not rare. Studies show that 20% to 45% of people who use supplements and prescription drugs together face potential interactions. You should always review your medications and supplements with your healthcare provider to avoid severe drug interactions and drug-condition interactions.
Signs of Interactions

Recognizing the signs of supplement and medication interactions can help you avoid serious health problems. You should always watch for changes in your body or mind when you start a new supplement or medication. Some signs may appear quickly, while others develop over time. Knowing what to look for helps you act fast if a drug interaction occurs.
Physical Symptoms
Physical symptoms often give you the first clue that an interaction is happening. These symptoms can range from mild to severe. You should pay close attention to any new or unusual changes.
Allergic Reactions
Allergic reactions can happen with any supplement or medication. You might notice rashes, itching, swelling, or trouble breathing. These symptoms can signal a dangerous interaction. If you see these signs, seek medical help right away.
Bleeding or Bruising
Some drug interactions increase your risk of bleeding or bruising. For example, combining omega-3 supplements or turmeric with blood thinners can make you bleed more easily. You may notice nosebleeds, bleeding gums, or bruises that appear without reason.
Heart Rate Changes
Certain interactions can affect your heart. You might feel your heart racing, skipping beats, or pounding in your chest. St. John’s Wort mixed with antidepressants can cause a rapid heartbeat or high blood pressure. Always report these symptoms to your healthcare provider.
Here is a table showing common physical symptoms linked to specific supplement and medication interactions:
Supplement & Medication Interaction | Common Physical Symptoms Reported |
|---|---|
St. John’s Wort + Antidepressants | Rapid heartbeat, agitation, high blood pressure, hallucinations |
Omega-3 + Blood thinners | Increased risk of bleeding |
Vitamin D + Blood pressure medications | Constipation, nausea, vomiting (signs of high calcium) |
Turmeric + Anticoagulants | Increased risk of bleeding |
Kava + CNS depressants | Liver injury, drowsiness, slowed breathing |
Mental Symptoms
Drug interactions can also affect your mind. You should watch for changes in mood or thinking.
Mood Changes
You may feel more agitated or restless than usual. Some interactions, especially those involving supplements and antidepressants, can cause agitation or distress. These changes may be early signs of a serious problem like serotonin syndrome.
Confusion
Confusion or trouble thinking clearly can signal a dangerous interaction. You might feel disoriented or have trouble remembering things. These symptoms often appear with other signs, such as agitation or changes in heart rate.
Tip: If you notice sudden mood changes or confusion, contact your healthcare provider. These symptoms can mean a drug interaction is affecting your brain.
Emergency Signs
Some interactions can cause life-threatening symptoms. You need to know when to seek emergency help. Watch for these warning signs:
Emergency Sign Category | Examples of Life-Threatening Signs and Symptoms |
|---|---|
Neurological | Dizziness, confusion, seizures, serotonin syndrome (fever, fast heartbeat, muscle twitching) |
Cardiovascular | Irregular heartbeats, chest pain, arrhythmias, low blood pressure, electrolyte problems |
Bleeding Abnormalities | Unusual bruising, prolonged bleeding |
Renal Failure | Sudden kidney problems, changes in urination |
Hypoglycemia | Severe low blood sugar, shakiness, sweating, fainting |
Severe Allergic Reactions | Rashes, itching, swelling, trouble breathing |
CNS Depression | Extreme drowsiness, slow breathing, trouble waking up |
You should also watch for:
Dizziness, headaches, or sudden confusion
Chest pain or heart palpitations
Jaundice or dark urine
Severe nausea, vomiting, or stomach pain
Medication not working as expected
Severe fatigue or weakness
If you see any of these signs, get medical help immediately. Always tell your healthcare provider about all supplements and medications you use. Quick action can save your life when a drug interaction causes an emergency.
Check Interactions
You play a key role in preventing harmful drug interaction problems. Checking for interactions before starting any new supplement or medication keeps you safe. Use these steps to protect your health and avoid unexpected side effects.
Consult Healthcare Providers
Always tell your healthcare provider about every supplement, vitamin, and medication you use. Many people forget to mention over-the-counter products or herbal remedies, but these can cause serious drug interaction issues. Recent surveys show that healthcare professionals discuss supplement use with patients in only about 42% of visits. This means more than half of patients may not share important information, leaving their healthcare provider unaware of possible risks. You should bring a complete list of your medications and supplements to every appointment. This helps your healthcare provider spot potential problems and give you the best advice.
Tip: Write down all the supplements, vitamins, and medications you take. Share this list with your healthcare provider at every visit.
Use Drug Interaction Checkers
You can use a drug interaction checker to review your medications and supplements for possible problems. These online tools help you find out if your combination is safe. WebMD’s drug interaction checker is one of the most trusted options. Healthcare professionals recommend it because a licensed pharmacist reviews the information for accuracy. The tool explains what types of drug interaction might happen, what symptoms to watch for, and how to stay safe. You should use a drug interaction checker every time you add a new supplement or medication to your routine. This step gives you quick answers and helps you prepare questions for your healthcare provider.
Here is how you can use a drug interaction checker:
Enter the names of all your medications and supplements.
Review the results for any warnings or alerts.
Read about possible symptoms and what to do if you notice them.
Print or save the results to discuss with your healthcare provider.
Note: A drug interaction checker does not replace medical advice. Always confirm results with your healthcare provider.
Read Labels
Medication and supplement labels give you important safety information. Always read the label before taking any new product. Labels warn you about possible drug interaction risks, side effects, and when to call your healthcare provider. You will often see advice to avoid certain foods, drinks, or other supplements. Some labels highlight specific risks, such as interactions with St. John’s wort or Ginkgo biloba. You may also find warnings about allergies, pregnancy, or pre-existing conditions.
Common warnings on labels include:
Possible changes in how your body absorbs, breaks down, or removes a medication.
Side effects that may happen when you combine products.
Advice to consult your healthcare provider before mixing supplements and medications.
Reminders to keep a list of all your medications and supplements.
Cautions about not sharing medications or assuming over-the-counter products are always safe.
Alert: Never ignore label warnings. If you have questions, ask your healthcare provider or pharmacist for help.
By checking interactions with your healthcare provider, using a drug interaction checker, and reading labels, you lower your risk of dangerous side effects. These steps help you use every medication and supplement safely.
Safety Tips for Safe Medication Use
Keep a List
You should always keep an updated list of every supplement and medication you take. This list helps you and your healthcare providers spot possible interactions and avoid mistakes. Many people visit different doctors or pharmacies, so your records may be incomplete. When you keep a list, you give your providers the information they need to protect your safety.
Clinical studies show that sharing a complete list of supplements and medications improves your provider’s ability to manage your therapy and prevent adverse interactions. Pharmacists use these lists to check for problems and suggest safer schedules or alternatives. If you ever face an emergency, your list helps doctors act quickly and safely.
Tip: Write down the name, dose, and reason for each supplement and medication. Update your list every time you start or stop a product.
Supplements are often missed in medical records, which increases the risk of serious interactions.
Medication therapy management programs can help you review your list with a pharmacist for extra safety.
Communicate Regularly
You need to talk openly with your healthcare providers about all supplements and medications you use. Many providers do not ask about supplements, and patients may forget to mention them. Regular communication helps you avoid dangerous interactions and side effects.
Best practices include discussing why you take each supplement, how to use it, possible risks, and whether it works for you. Providers should ask about your supplement use and explain the benefits and risks. You should also ask questions about cost, effectiveness, and alternatives.
Both you and your provider play a role in safe medication use. More frequent and thorough discussions lead to better decisions and improved safety. Providers may need extra training to cover all topics, so you should prepare questions before your visit.
What to Discuss With Your Provider | Why It Matters |
|---|---|
All supplements and medications | Prevents interactions and errors |
Reasons for use | Ensures correct treatment |
Risks and side effects | Improves safety |
Effectiveness | Guides therapy choices |
Costs and alternatives | Supports informed decisions |
Note: Providers may not cover every topic, so you should bring up anything that concerns you.
Avoid Self-Medicating
You should never mix supplements and medications without professional guidance. Self-medicating can lead to serious health risks. Many people try to treat themselves, but this can cause dangerous drug interactions, incorrect dosages, or missed diagnoses.
If you self-medicate, you may delay getting the right treatment. You could mask symptoms of a serious disease or make your condition worse. Herbal supplements sometimes contain hidden ingredients that interact with prescription drugs or worsen existing problems.
Older adults who take many medications face higher risks of adverse reactions. Some herbal products can interact with anesthetics, blood thinners, or cancer treatments. Quality concerns also exist, such as contamination or mislabeling. Pregnant women should be especially careful, since supplement safety is often unclear.
Incorrect self-diagnosis leads to poor treatment.
Delays in seeking medical attention can worsen your health.
Mixing supplements and medications without advice increases the risk of dangerous interactions.
Allergic reactions and side effects may happen unexpectedly.
Mental health self-medication is risky and can make conditions worse.
Alert: Always consult your healthcare provider before starting any new supplement or medication. Professional advice keeps you safe and helps you avoid serious problems.
Medical Disclaimer: This information is for educational purposes only. You should always talk to a healthcare professional before making decisions about supplements or medications.
Store Safely
Storing your supplements and medications the right way protects your health and prevents dangerous mistakes. Many people choose storage spots based on convenience or child safety, but you also need to think about temperature, humidity, and light. These factors can change how well your medications work and may even cause harmful interactions.
Key steps for safe storage:
Choose the right location:
Store your medicines in a dry, cool place. Bathrooms often have too much moisture, which can damage pills and capsules. A bedroom drawer or a high shelf in a closet works better.Keep medicines out of reach:
If you have children or pets at home, always use childproof containers and store medications in locked or hard-to-reach places. Medications left on countertops or in purses can lead to accidental ingestion and emergency room visits.Use original containers:
Keep all supplements and medications in their original packaging. These containers protect against light and moisture. They also have important labels and instructions you might need.Monitor for changes:
Check your medications for any signs of damage, such as changes in color, smell, or texture. If you notice anything unusual, ask your pharmacist before taking them.Dispose of old or unused medications:
Expired or discontinued products can be dangerous. Remove them from your home as soon as possible. Use medicine take-back programs or follow disposal instructions on the label. Never flush medications unless the label says it is safe.Ask your pharmacist:
Pharmacists can teach you about proper storage and disposal. They can also help you spot signs of medication degradation and answer questions about safe use.
Tip: Always take your medicine in a well-lit, clean area. This helps you avoid mistakes and keeps your routine safe.
Storage Tip | Why It Matters |
|---|---|
Dry, cool place | Prevents breakdown from heat and moisture |
Childproof location | Reduces risk of accidental ingestion |
Original containers | Protects from light, moisture, and confusion |
Prompt disposal | Prevents accidental use and harmful interactions |
Pharmacist guidance | Ensures correct storage and disposal |
You play a big role in medication safety by storing your products correctly. Good storage habits help you avoid accidental interactions, keep your medicines effective, and protect everyone in your home.
Medical Disclaimer: This information is for educational purposes only. Always consult your healthcare provider or pharmacist for advice about supplements or medications.
What To Do If You Suspect Interactions
If you think you are experiencing interactions between a supplement and a medication, you need to act quickly and carefully. Recognizing and responding to interactions can protect your health and prevent serious problems. Here’s what you should do:
Immediate Steps
When you suspect interactions, follow these steps to stay safe:
Use a trusted online interaction checker like Drugs.com, WebMD, or Medscape. Enter all supplements and medications you take to see if any interactions appear.
If the checker shows a moderate or major interaction, or if you feel unsure about the results, contact your healthcare provider or pharmacist for advice.
Do not stop any medication suddenly. Always wait for professional guidance before making changes to your routine.
When you speak with your provider, tell them which interaction checker you used and what interactions were flagged. This helps them give you the best advice.
Keep an up-to-date list of all your supplements and medications. This list helps your provider spot interactions more easily.
Try to use one pharmacy for all your prescriptions and supplements. Pharmacists can help catch interactions that might be missed elsewhere.
Tip: Write down any new symptoms you notice. This record can help your provider understand if interactions are causing your problems.
When to Seek Help
Some interactions can cause emergencies. You need to know when to get help right away. Call emergency services if you notice any of these signs:
Uncontrollable bleeding or a wound that will not stop bleeding after 15 minutes.
Unconsciousness, seizures, or sudden confusion.
Signs of shock, like weakness, bluish lips, clammy skin, or paleness.
Chest pain, irregular heartbeat, or trouble breathing.
If you suspect an overdose or a very serious reaction, call emergency services immediately. While waiting for help, check the person’s airway, breathing, and pulse. Begin CPR if needed. Place an unconscious but breathing person in the recovery position. Try to identify all substances taken and share this information with emergency personnel.
Alert: Never ignore severe symptoms. Quick action can save a life when interactions become dangerous.
Report and Document
After you manage the immediate situation, you should document and report the suspected interactions:
Write down everything about the event. Include the names and doses of all supplements and medications, the symptoms you experienced, and when they started.
Collect details like lot numbers, manufacturer names, and any other information from the product labels.
Report the interaction to your healthcare provider and, if possible, to regulatory bodies such as the FDA. You can use the MedWatch program to submit a report online, by phone, fax, or mail.
Include as much detail as possible in your report. This helps experts find patterns and improve safety for everyone.
Even if you are not sure the interaction caused the problem, reporting helps track new or unexpected interactions.
Note: Reporting suspected interactions helps protect others and improves the safety of supplements and medications for everyone.
Medical Disclaimer: This information is for educational purposes only. It does not replace medical advice. Always consult a healthcare professional before making decisions about supplements or medications.
To use supplements and medications safely, you should:
Consult your healthcare provider before starting anything new.
Store and dispose of products properly.
Staying informed and talking regularly with your healthcare team helps you avoid harmful interactions. You take control of your health by making smart, safe choices.
Medical Disclaimer: This information is for educational purposes only. Always consult a healthcare professional before making decisions about supplements or medications.
FAQ
Can supplements interact with prescription medications?
Yes, supplements can change how your body absorbs or processes medications. You may experience reduced effectiveness or increased side effects. Always tell your healthcare provider about every supplement you use.
How do I know if I am having a supplement-drug interaction?
You may notice new symptoms like rash, bleeding, confusion, or heart changes. Use a drug interaction checker and contact your healthcare provider if you feel unwell after starting a new supplement.
Should I stop taking supplements before surgery?
You should tell your doctor about all supplements before surgery. Some supplements increase bleeding risk or affect anesthesia. Your doctor may ask you to stop certain products several days before your procedure.
Are herbal supplements safer than vitamins?
Herbal supplements can cause strong interactions, just like vitamins. You should not assume herbs are safer. Both types can affect medications. Always check with your healthcare provider before starting any supplement.
What is the best way to keep track of my supplements and medications?
Write a list with names, doses, and reasons for each product. Update your list when you start or stop anything. Share this list with your healthcare provider at every visit.
Can food affect how my supplements or medications work?
Yes, some foods change how your body absorbs or breaks down medications and supplements. Grapefruit juice and foods high in vitamin K are common examples. Read labels and ask your healthcare provider for advice.
Where can I check for supplement and medication interactions online?
You can use trusted sites like WebMD, Drugs.com, or Medscape. Enter your medications and supplements to see possible interactions. Always confirm results with your healthcare provider.
Medical Disclaimer:
This information is for educational purposes only. It does not replace medical advice. You should consult a healthcare professional before making decisions about supplements or medications.